
At a glance:
- Covid-19 patients at LGH and WellSpan now number over 100
- Hospitals prepared for surge continuing into December
- UPMC silent on its patient count
- Death toll rises slowly, below rate of serious cases, an indicator of improved care
- Among those who have tested positive, about 1 in 30 has died
- New infections highest in Lancaster city and suburbs
- Many staff ill at nursing homes, but few residents sick, no deaths
- Data on many homes missing from state health website
Overview
The COVID-19 pandemic sharply increased its impact on Lancaster County residents in the past week, sending a record number of patients to area hospitals. New infections also hit their highest level since the beginning of the pandemic in March.
But, in contrast to some cities and counties in other states, Lancaster County hospitals still have sufficient drugs, equipment and – most importantly – hospital bed capacity. Their greatest challenge is maintaining adequate staffing levels.
Hospitalizations
The number of hospitalized COVID-19 patients has more than doubled in the first three weeks of November.
Between Nov. 1 and 21, the number of patients hospitalized at Penn Medicine Lancaster General Health and Wellspan Health Ephrata increased 150% from 40 to 101.
The low point in hospital cases occurred Sept. 20, when just seven patients were in the two hospitals.
The previous high was 56 hospitalizations on April 28.
At a LGH board meeting Thursday, Dr. Michael Ripchinski said the hospital used the lull in past months to build stocks of pharmaceuticals and personal protection gear so that it has adequate supplies for this new wave of illness. The hospital also has contingency plans to provide additional beds beyond those in its current COVID-19 units, should the need arise.
His remarks on preparations echoed those of Ryan Coyle, a spokesman for Wellspan Health Ephrata, who last week said that hospital is prepared to double its ICU beds, if needed, and can shift patients among its six regional hospitals if a localized outbreak pushes any one hospital to capacity.
The county’s third hospital, UPMC Lititz, has not been willing to provide information on the number of its COVID-19 patients. Spokeswoman Kelly McCall did say the hospital is seeing an increase in COVID positive patients, but fewer needing ICU care. The UPMC system has “robust” plans in place to increase capacity, using transfers of patients, if necessary, among its 40 facilities, she said.
A further indicator of the ability of county hospitals to meet the surge in COVID-19 patients comes from the state Health Department. Today its dashboard shows that 119 medical beds, 11 ICU beds and 14 airborne isolation beds remain available in the county, according to filings it receives daily from county hospitals.
Deaths
Twenty-seven county residents died here from COVID-19 during the first three weeks of this month. That rate – slightly more than one person per day – is far below what occurred in April, the peak month for deaths here, when about six county residents died each day.
Still, the death toll is already more than double the rate in September, when the pandemic had receded and just 13 died in the county during the entire month.
So far as age, one victim each was in his or her 40s, 50s and 60s. Nine were in their 70s, and the remainder were age 80 and above.
Geographically, there were three victims each in Lititz, West Donegal, East Lampeter and Manheim townships. There were two each in West Lampeter and Ephrata townships. One each died in Earl, East Earl, West Earl, West Hempfield, Paradise, Penn, Rapho, Salisbury, Warwick and Lancaster townships, as well as one in Akron borough.
There were no virus-related deaths in 43 (54%) of the county’s 60 municipalities.
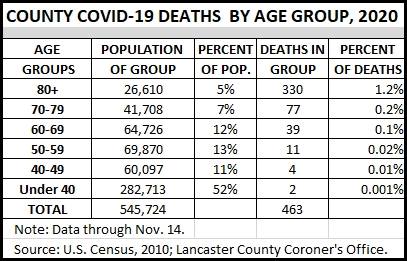
Risk
Since the pandemic began here in late March, COVID-19 has taken the lives of 1.3% percent of the county’s population age 80 and above. It’s struck down 0.2% of those in their 70s and 0.1% of those in their 60s. No one under age 25 has succumbed to the virus.
The risk of catching the virus and dying from it remains very low for those under age 80.
HOWEVER, if a person does catch the virus, the risk of death increases significantly. Since March, there have been 13,920 confirmed cases of COVID-19 and 475 virus-related deaths here.
In other words, about 1 in 30 individuals (3.4%) who tested positive for the virus subsequently died from it.
New cases (Positive COVID-19 tests)
Lancaster County hospitals, clinics and doctors reported 3,891 positive COVID-19 tests during the first three weeks of November, almost double the total of October (1,968).
A third of the cases (32%), about 1,250, occurred among residents of Lancaster city and its suburbs.
Three borough-related ZIP code areas also had increased positive tests: Lititz (17543) 346 cases, Ephrata (17522) 264 cases and Elizabethtown (17022) 215 cases.
To complete the case rundown:
- Four ZIP code areas – Manheim, Mount Joy, Denver and New Holland – had between 100 and 200 new cases in the past three weeks.
- Eight areas – Columbia, Leola, Millersville, Quarryville, Willow Street, Mountville, Stevens, and Marietta – had 50 to 100 new cases.
- The other 26 areas had fewer than 50 cases. Smoketown had none.
On a per capita basis, the picture is different. Tiny Terre Hill (pop. 951) has a rate of 20 cases per 1,000 residents this month. The next highest areas of per capita infection were: Leola (9.4), Manheim (8.8), New Holland (8.7), and Mount Joy and Mountville (both 8.3).
The Lancaster ZIP code areas had per capita rates ranging from 7.7 to 8.3 per 1,000 residents.
More cases, fewer deaths
The landscape of treatment and recovery for COVID-19 patients had changed substantially in the past nine months.
In April, when most patients were going to LGH, the patient count in that hospital rose from 25 to 39 in the first three weeks of the month. During that same time period, 112 county residents died, most of them in nursing homes who never got to the hospital.
In the same time span this month, the patient count has risen to 101, 2½ times the April caseload and yet the death toll is about a quarter of what it was in that first full month of the pandemic.
That dramatic change illustrates how much doctors and nurses have learned about treatment of the disease in the past eight months.
At the LGH board meeting, Dr. Joseph M. Kontra, chief of Infectious Diseases, said the hospital staff now uses remdesivir and dexamethasone, antiviral medications, for COVID-19 patients. They also use convalescent plasma (blood with antibodies donated by recovered patients) and Regeneron, a monoclonal antibody medication to help patients build their immune systems.
Former patients have been generous with plasma donations, Dr. Kontra said, and the hospital has more than 100 units stored for future use.
Comparison to flu
Is the COVID-19 virus greatly different from seasonal flu of past years?
County and national statistics suggest that it is.
In the 2019 Lancaster County Coroner’s Report, Dr. Stephen Diamantoni reported that 89 area residents died of all respiratory illnesses, which would include flu. In the 10¾ months of this year, 475 have died just of COVID-19.
In the 2019-20 flu season, 22,000 Americans died of the influenza virus, the Center for Disease Control says. In 2017-18, an estimated 61,000 died.
In comparison, since March, an estimated 257,000 people have died in the U.S.
Nursing and personal care homes
In spring, nursing and personal care homes were the epicenter of the pandemic. Scores of residents died as nursing personnel and health officials struggled to come to grips with a new virus especially harmful to the elderly.
Nursing homes quickly adopted stern, now well-known measures to stop the virus spread. They quarantined residents, tested staff daily, secured protective equipment, and adopted numerous CDC-recommended sanitation procedures.
Now the status of area congregate homes is much improved.
So far this month, nursing homes reported only three new cases – and no deaths – among their residents. There were, however, 36 new cases among staff members.
This positive picture, however, may be distorted by the absence of some facility reports on the state Health Department website. This week, the state site indicated that eight of 32 nursing homes had not filed a report:
- Kadima Rehabilitation & Nursing, Lititz
- Landis Homes, Lititz
- Manorcare Health Services, Lancaster
- Newport Meadows Health and Rehabilitation Center, Christiana
- Quarryville Presbyterian Retirement Community, Quarryville
- Rose City Nursing and Rehabilitation at Lancaster
- Susquehanna Valley Nursing & Rehabilitation Center, Columbia
- Zerbe Sisters Nursing Center, Narvon.
Reports for four facilities have not appeared on the state website since the pandemic began: Manorcare, NewPort Meadows, Rose City and Susquehanna Valley Nursing.
Similarly, personal care homes reported only one new resident case, no deaths and six new cases among staff. But there are 21 of 57 personal care homes for which there are no reports.
Nate Wardle, a spokesman for the state Health Department, said health officials are working with nursing homes to ensure that they report accurate, cumulative data on their residents.
Some facilities have had issues using the state’s data reporting system, he acknowledged, adding that department officials “are continuing to work to get as many facilities as possible reporting.”
This report has been compiled from records of the Lancaster County Coroner’s Office, the state Health Department, Penn Medicine Lancaster General Health and WellSpan Health Ephrata by researcher Erica Runkles, sociologist Mary Glazier and journalist Ernest Schreiber.
Note 1: The full board meeting of Penn Medicine Lancaster General Health can be viewed here. The COVID-19 discussion begins at 33 minutes, 45 seconds.
Note 2: The data charts of county deaths, hospitalizations and cases maintained by researcher Erica Runkles can be viewed here.
Hospitalizations
The number of hospitalized Covid-19 patients – the second most important index of the pandemic’s health impact –has nearly doubled in the first two weeks of November.
Between Nov. 1 and 14, the number of patients hospitalized at Penn Medicine Lancaster General Health and Wellspan Health Ephrata rose from 40 to 77. (As of Monday, Nov. 16, there were 80.)
The number of patients at LGH alone – 66 – is higher than at any time since March. The previous high was 56 hospitalizations on April 28.
According to state Health Department, the county has 80 medical beds, 18 intensive care unit beds and 11 airborne isolation, a total of 109 beds. If the health department’s report is accurate, county hospitals were at about 70% of capacity for COVID-19 patients on Saturday (73% on Monday).
Those numbers, however, appear to reflect the hospitals’ traditional, pre-pandemic capacity and do not include measures the facilities have taken since March to provide additional beds for COVID-19 patients.
Ryan Coyle, a spokesman for Wellspan Health, said Ephrata hospital in fact has 122 acute care beds, including 10 critical care (ICU) beds. If necessary, the hospital can expand those 10 ICU units to accommodate 20 critically ill patients. WellSpan Health has six hospitals, he added, and if one hospital reaches capacity, patients can receive care at any of the others.
John Lines, a LGH spokesman, was asked to confirm that facility’s capacity for COVID-19 patients. We will update this report if and when that information becomes available.
Whatever the LGH response, it appears clear that hospital capacity here is significantly above that reported by the Health Department.
New cases (Positive Covid-19 tests)
Lancaster County hospitals, clinics and doctors reported 2,164 positive COVID-19 tests during the first two weeks of November, more than the total in October (1,968) and September (1,279).
About one-third (32%) of those cases occurred among residents of Lancaster city and its suburbs. The western metro area (17603 ZIP code) had the highest case count at 253. The southeastern metro area (17602) had 239 cases, followed by the northern metro area (17601) with 194 cases.
Three borough-related ZIP code areas also had increased positive tests: Lititz (17543) 206 cases, Ephrata (17522) 167 cases and Elizabethtown (17022) 115 cases.
Shane Weaver, president of Lititz borough council, said he knows of no obvious reason for the rising number of cases in that town. People wear masks in the shopping district, he said, and there has been no report of an outbreak. One possibility, he said, might be cases at the five nursing homes that are within the Lititz postal area.
Nursing and personal care homes also may account for the rise in cases in other towns, but state Health Department reports on those facilities are incomplete, making such a determination impossible.
To complete the case rundown:
- Five ZIP code areas – Manheim, Mount Joy, Denver, New Holland and Leola – had between 50 and 100 new cases in the past two weeks.
- Ten ZIP code areas – Quarryville, Columbia, Mountville, Millersville, Willow Street, Marietta, Stevens, Narvon, Landisville and East Earl – had 20 to 49 cases.
- The other 23 areas had fewer than 20 cases. Smoketown had none.
For perspective, in all these areas, about three to five residents out of every 1,000 (fewer than 1%) tested positive – during the past two weeks. And, as Dr. Anthony Fauci, the CDC’s top pandemic expert, has stated, about 80% of those who test positive do well without any specific medical treatment.
This report has been compiled from records of the Lancaster County Coroner’s Office and the state Health Department by researcher Erica Runkles, sociologist Mary Glazier and journalist Ernest Schreiber. The data chart maintained by Erica Runkles can be viewed here.





